problem with extending the approach to other kinds of tissue-specific stem cells is that it has not always been easy to find the kind of tissue-specific stem cell you want.
Transplanted Stem Cells Reverse Juvenile Diabetes in Mice
Very promising experiments carried out in 2000 by Dr. Ammon Peck and a team of researchers at the University of Florida concerns a particularly vexing problem, that of type-1 or juvenile diabetes. A person with juvenile diabetes lacks insulin-producing pancreas cells, because their immune system has mistakenly turned against them and destroyed them. They are no longer able to produce enough insulin to control their blood sugar levels and must take insulin daily. Adding back new insulin-producing cells called islet cells has been tried many times, but doesn’t work well. Immune cells continue to destroy them.
Peck and his team reasoned, why not add instead the stem cells that produce islet cells? They would be able to produce a continuous supply of new islet cells, replacing those lost to immune attack. Because there would always be cells to make insulin, the diabetes would be cured.
No one knew just what such a stem cell looked like, but the researchers knew they come from the epithelial cells that line the pancreas ducts. Surely some must still lurk there unseen. So the research team took a bunch of these epithelial cells from mice and grew them in tissue culture until they had lots of them.
Were the stem cells they sought present in the cell culture they had prepared? Yes. In laboratory dishes the cell culture produced insulin in response to sugar, indicating islet cells had developed in the growing culture, islet cells that must have been produced from stem cells. Now on to juvenile diabetes. The scientists injected their cell culture into the pancreas of mice specially bred to develop juvenile diabetes. Unable to manufacture their own insulin because they had no islet cells, these diabetic mice could not survive without daily insulin. What happened? The diabetes was reversed! The mice no longer required insulin.
Impatient to see in more detail what had happened, the researchers sacrificed the mice and examined the cells of their pancreas. The mice appeared to have perfectly normal islet cells.
One might have wished the researchers waited a little longer before terminating the experiment. It is not clear whether the cure was transitory or long term. Still, there is no escaping the conclusion that injection of a culture of adult stem cells cured their juvenile diabetes.
While certainly encouraging, a mouse is not a human, and there is no guarantee the approach will work in humans. But there is every reason to believe it might. The experiment is being repeated now with humans. People suffering from juvenile diabetes are being treated with human pancreatic duct cells obtained from people who have died and donated their organs for research. No ethical issues arise from using cells of adult organ donors, and initial results look promising.
Transplanted stem cells may allow us to replace damaged or lost tissue, offering cures for many disorders that cannot now be treated. Current work focuses on tissue-specific stem cells, which do not present the ethical problems that embryonic stem cells do.
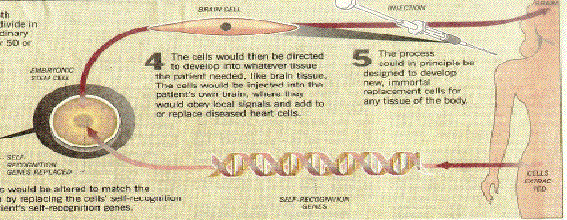 Figure 24b
Figure 24b